Metformin: is it an anti-aging pill?
- Published in Primary Prevention & Lifestyle
- Written by Monica

The science of aging is moving forward as scientists are elucidating the biology of aging. The ultimate goal is to develop treatments that delay aging, and in so doing, delay the development of aging-related diseases.[1]
Aging is the greatest risk factor for the majority of chronic diseases that are driving morbidity and health costs [2], but the aging process can be delayed with lifestyle (exercise and nutrition), genetics, and pharmacologic approaches.[3-8]
The so called “geroscience hypothesis” (“gero” is short for gerontology, which is the scientific study of the process of aging and its consequences) holds that treatments that are targeting fundamental processes of aging may delay, prevent, alleviate, or reverse a wide range of diseases and conditions for which age is the primary non-modifiable risk factor.[1] Interventions that target fundamental aging processes have the potential to transform human health and health care.[9]
Excitement is now high because time has come for the first study to test the effect of metformin on aging-related outcomes in humans and see if it qualifies as an "anti-aging pill"...
Article Tags
Caloric Restriction for anti-aging and longevity - does it work in non-obese humans?
- Published in Diet, Nutrition & Supplements
- Written by Monica

If you are following the anti-aging news, you’ve heard about the supposed benefits of chronic calorie restriction for increasing longevity. These claims are based on research done in various species such as flies, worms and mice.
Here I will explain that chronic calorie restriction makes it impossible to implement and reap the health benefits of an active lifestyle with regular exercise, and causes severe health consequences for humans.
While animal studies can and do shed light on what’s going on at mechanistic level, we have to be very careful and resist the temptation to extrapolate results from animal experiments to humans.
Here I will make the case that chronic calorie restriction actually counteracts the prospects of a healthy vital long life.
Article Tags
Waist-to-Height Ratio as a Screening Tool for Testosterone Deficiency
- Published in Testosterone Replacement Therapy
- Written by Monica
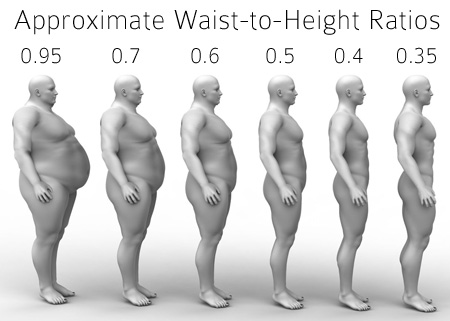
A bidirectional relationship exists between excess body fat, and/or belly fat, and testosterone levels in men. That is, excess body (belly) fat decreases testosterone levels and may cause testosterone deficiency, and low testosterone levels increases body (belly) fat.[1-4] I covered this in-depth in a previous article “Testosterone and Fat Loss - the Evidence”.
In “Keep your waist to less than half your height” I introduced the waist-to-height ratio and explained that it is a better tool for predicting health outcomes and mortality than is waist circumference alone. I have also covered the association between a large waist (i.e. belly) and reduced testosterone levels in "Young Men, Waist, Testosterone and Erectile Function: Low-T is not only an old man's issue".
Here I will summarize research showing that the waist-to-height ratio can also be used as a screening tool for testosterone deficiency.
Article Tags
Young Men, Waist, Testosterone and Erectile Function: Low-T is not only an old man's issue
- Published in Waist - Abdominal Obesity
- Written by Monica

Most people, including traditional doctors, think that testosterone deficiency is an old man’s issue. This is very wrong! Actually, an excess amount of body fat can cause a man’s testosterone levels drop to as much as 10 years of aging.[1]
Several studies have demonstrated that too much body fat is associated with reduced testosterone levels independent of aging.[2-4]
Low levels of testosterone (both total and free testosterone) are a consistent feature among young men below 40 years of age with metabolic syndrome, the hallmark of which is an enlarged belly.[5]
Young men (20–39 years) with the lowest baseline total testosterone levels have the highest risk of developing cholesterol and blood fat abnormalities (dyslipidemia). [6] Compared to age-matched men with the highest baseline total testosterone levels of 663 ng/dL or higher, those with the lowest baseline total testosterone levels of 418 ng/dL or below had up to a twofold greater risk of developing an adverse lipid profile 5 years later, which in turn could contribute to future risk of cardiovascular disease.[6]
Thus, testosterone deficiency clearly has health implications also for younger men. But how much does your belly actually impact your testosterone levels… and erectile function?
Article Tags
Keep your waist to less than half your height - for health and physical attractiveness
- Published in Waist - Abdominal Obesity
- Written by Monica

In a previous article “Watch Your Belly – not just to look good!” I summarized research showing that an expanded belly is a ticking health bomb and manifestation of deteriorating vitality, as well as reduced physical attractiveness.
Measuring your waist circumference is a good starting point to see where you stand (i.e. to get your baseline) and monitor your progress with exercise and healthier eating. And esthetically, your waist measure tells a lot.
Nevertheless, accumulating research shows that health outcomes are more strongly associated with the ratio of your waist to your height, i.e. the waist-to-height ratio. The waist-to-height ratio is simply the ratio of your waist circumference to your height (abbreviated WHtR). To stay (or become) healthy, as well as physically attractive, make sure your waist circumference is less than half your height.
Video Summary: Testosterone Deficiency and Treatment - International Expert Consensus Resolutions
- Published in Testosterone Replacement Therapy
- Written by Monica

In a previous article "Testosterone Deficiency and Treatment - the FACTS" I presented the conclusions from an International Expert Consensus Conference on Testosterone Deficiency and Its Treatment.[1]
Here I summarize the key points, and link to a video summary by Dr. Abraham Morgentaler, an internationally renowned testosterone scientist and clinician.
Article Tags
Watch Your Belly – not just to look good!
- Published in Waist - Abdominal Obesity
- Written by Monica

Over the past two decades it has been established beyond any doubt that the amount of fat around the waist (aka abdominal fat and visceral fat) is at least as important, if not more important, than the total amount of body fat in predicting and /or causing complications that have been traditionally associated with overweight/obesity.[1]
Abdominal obesity is a strong risk factor for cardiovascular disease independent of BMI (a proxy for obesity) [2, 3] and is thought to affect disease risk through increased insulin resistance.[4, 5] Actually, the common development of insulin resistance with aging is caused by growing bellies, rather than aging per se.[6] Notably, normal-weight abdominal obesity is associated with higher mortality than generalized obesity (as defined by BMI).[7]
An enlarged belly is an especially strong indicator of metabolic risk in men.[8, 9] People with large a waist circumference – i.e. those having a belly - have an increased risk of cardiovascular disease, diabetes and cancer, compared to those with smaller waist circumferences, regardless of BMI. [10-14] Your waist also impacts your longevity, which I covered in a previous article "Watch Your Waist - it may shorten your life!"
And your belly can interfere with your sex life...
Article Tags
Testosterone Deficiency and Treatment - the FACTS
- Published in Testosterone Replacement Therapy
- Written by Monica

Testosterone deficiency and treatment is a very misunderstood and controversial topic among scientists, regulatory agencies (such as the FDA and EMA) and doctors, as well as the popular media.
On October 1, 2015, an international expert consensus conference about testosterone deficiency and its treatment was held in Prague, sponsored by King’s College London and the International Society for the Study of the Aging Male (ISSAM). The impetus for this meeting was to address the widespread misinformation and confusion about testosterone deficiency and testosterone therapy.[1]
The ultimate goal of this consensus conference was to document what is true or untrue about testosterone deficiency and testosterone therapy, to the best degree possible based on existing scientific and clinical evidence.
There were 18 experts from 11 countries on 4 continents. Specialties included urology, endocrinology, internal medicine, diabetology, and basic science research. Experts were invited on the basis of extensive clinical experience with testosterone deficiency and its treatment and/or research experience.
The final consensus on several key issues related to testosterone therapy was published in the form of 9 resolutions (i.e. firm decisions), coupled with expert comments.[2] These are summarized in table 1.
Article Tags
Testosterone Replacement Therapy
- Published in Testosterone Replacement Therapy
- Written by Monica

When you see the term “testosterone,” we typically associate it with masculinity and men. However, women generate testosterone too. So, what exactly is testosterone? Testosterone is a steroid hormone that plays a significant role in the male sperm production and produced in women’s ovaries in much smaller amounts. Rising levels of testosterone stimulates physical and chemical changes for boys and men such as increased muscle, pubic hair growth, deeper lengthened vocal chords, and increased sexual desire.
Blood Testing - why?
- Published in Primary Prevention & Lifestyle
- Written by Monica
More...
- Real-life experience of continuous long-term testosterone therapy on anthropometric, endocrine and metabolic parameters for up to 10 years
- Remnant Cholesterol and non-HDL – What’s that? Why bother?
- Survival and cardiovascular events in men on testosterone treatment
- Everything We Learned About TESTOSTERONE Is WRONG - video presentation by Dr. Morgentaler




