Waist-to-Height Ratio as a Screening Tool for Testosterone Deficiency
- Published in Testosterone Replacement Therapy
Young Men, Waist, Testosterone and Erectile Function: Low-T is not only an old man's issue
- Published in Waist - Abdominal Obesity

Watch Your Belly – not just to look good!
- Published in Waist - Abdominal Obesity

Real-life experience of continuous long-term testosterone therapy on anthropometric, endocrine and metabolic parameters for up to 10 years
- Published in Testosterone Replacement Therapy
Effects of long-term testosterone treatment on weight loss and waist size in obese men - is TRT the next obesity treatment?
- Published in Testosterone Replacement Therapy
Testosterone Therapy Prevents Gain in Intra-Abdominal Fat and Counteracts Loss of Muscle in Non-Obese Aging Men
- Published in Testosterone Replacement Therapy

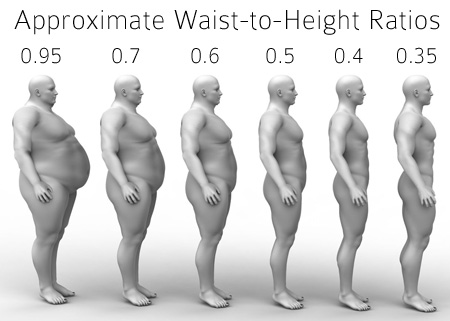
Watch Your Waist - it may shorten your life!
- Published in Waist - Abdominal Obesity

Your waistline not only makes or breaks your esthetic appearance; if you belly gets too large, it may greatly jeopardize your health and even longevity.
Waist circumference strongly correlates with abdominal obesity and is the most commonly used measure of body fat distribution.[1, 2] Many studies have found enlarged waist circumferences to be associated with all-cause mortality, in most cases independently of general obesity.[3-11]
Abdominal obesity (aka visceral obesity) appears to be more strongly associated with multiple chronic diseases than is gluteo-femoral obesity (fat deposition around the butt and thighs).[1] Increased waist circumference confers a health risk even in normal weight people.[12]
A notable large study investigated the association of waist circumference with mortality using intuitive 2 in (5 cm) increments for men and women, and also evaluated risk within narrow categories of body fatness (BMI). In addition, the study estimated years of life lost due to a large waist circumference.[13]
Testosterone Replacement Therapy (TRT) in Testosterone Deficient men - effects on fat loss, waist reduction and metabolic syndrome components
- Published in Testosterone Replacement Therapy

Testosterone deficiency in men, aka hypogonadism, is associated with increased total and abdominal fat mass, and reduced muscle mass, which negatively impacts body composition.[1, 2] This contributes to development of risk factors like insulin resistance, chronic inflammation, and atherogenic dyslipidemia (a triad of increased blood levels of small, dense LDL particles and triglycerides, and decreased levels of HDL particles), which increase the risk for cardiovascular disease, metabolic syndrome and diabetes.[1, 3-16]
Previous studies have shown that testosterone replacement therapy ameliorates these risk factors in testosterone deficient (hypogonadal) men; it increases insulin sensitivity [17-20] and HDL (the "good" cholesterol) [9, 10, 20, 21], and reduces waist circumference [9, 20, 22], fasting blood glucose [9, 20] triglycerides (blood fats)[9], LDL (the "bad" cholesterol) [19, 22-24], and several inflammatory markers.[17, 25]
A 2011 meta-analysis concluded that testosterone replacement therapy improves metabolic control, as well as reduces abdominal obesity.[9] Many studies have shown that testosterone replacement therapy in hypogonadal men increases muscle mass and reduces fat mass.[19, 26-32] Further, adding testosterone (50 mg/day for 1 year, administered as a transdermal gel) to a diet and exercise program results in greater therapeutic improvements of glycemic control and reverses the metabolic syndrome.[20]
Testosterone also has direct (non-obesity mediated) beneficial effects on many metabolic and cardiovascular risk factors [12, 33-37], and reduces death risk independently of body fat status.[38] In line with all these effects, low testosterone levels are associated with increased risk of cardiovascular complications [39], and all-cause and cardiovascular disease death [40-42]. Low testosterone may thus be a predictive marker for men at high risk of cardiovascular disease.[41] In a group of men aged 50-91 who were followed for 20 years, it was found that men whose total testosterone levels were in the lowest quartile (241 ng/dl or lower) were 40% more likely to die than those with higher levels, independent of age, adiposity, lifestyle or presence of cardiovascular risk factors.[38]
Thus, treatment of testosterone deficient men with testosterone has demonstrated considerable health benefits. Despite this, critics state that most of the studies on testosterone replacement therapy were too small. They also argue that the studies were of too short duration (most of them lasting 6-12 months), and that the long-term effects of testosterone on body composition are not known.
Two 5 year long studies were just published that addressed the duration and small study size shortcomings in previous research...
Effects of 6-year Long-Term Testosterone Replacement Therapy (TRT) in Patients with ‘‘Diabesity’’
- Published in Testosterone Replacement Therapy

March 6th 2014 FDA approved Aveed for treatment of male hypogonadism, aka testosterone deficiency.[1] Aveed is a long-acting form of injectable testosterone called testosterone undecanoate. In Europe, testosterone undecanoate (under the name Nebido) has a long successful TRT track record for treatment of testosterone deficiency and its consequences (especially obesity, the metabolic syndrome and diabetes).[2-16]
In contrast to shorter acting forms of testosterone (e.g. cypionate), testosterone undecanoate only needs to be injected every 6 to 12 weeks, and thereby offers practical benefits to patients. (Comment: for Nebido (1000 mg per 4 ml) the initial interval is 6 weeks, followed by intervals of 10-14 weeks; for Aveed (750 mg per 3 ml) the initial interval is 4 weeks, followed by 10-week intervals).
Five days after the FDA approval a notable and impressive 6-year long TRT study was published, confirming the health benefits of TRT that have previously been found in shorter term studies... [44]



