Testosterone treatment is NOT associated with risk of adverse cardiovascular events – the RHYME study
- Published in Testosterone Replacement Therapy
It is well-documented that testosterone therapy effectively restores testosterone levels in hypogonadal men and improves many health outcomes, such as quality of life [1-4], libido [4, 5], metabolic parameters [5-9] and body composition.[4, 5, 9, 10]
However, a few conflicting studies raised concerns about the cardiovascular safety of testosterone therapy [11, 12], which in 2015 prompted the FDA to issue warnings to physicians and patients about potential cardiovascular risks of testosterone therapy.
In contrast, the European Medicines Agency (EMA) acknowledged the flaws of the conflicting studies and concluded that there is no consistent evidence of harm associated with testosterone therapy, regardless of mode of delivery.[13]
Here I summarize the cardiovascular results of the notable RHYME (The Registry of Hypogonadism in Men) study, which contrary to prior clinical trials, enrolled men with a wide range of comorbid illnesses and cardiovascular risk factors.[14] The aim was to evaluate the safety of testosterone therapy in a sufficiently diverse population to reflect real-world, clinical experience.[14]
Waist-to-Height Ratio as a Screening Tool for Testosterone Deficiency
- Published in Testosterone Replacement Therapy
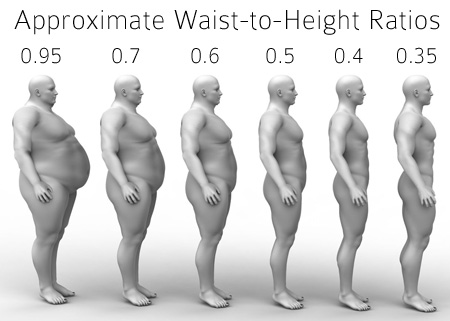
A bidirectional relationship exists between excess body fat, and/or belly fat, and testosterone levels in men. That is, excess body (belly) fat decreases testosterone levels and may cause testosterone deficiency, and low testosterone levels increases body (belly) fat.[1-4] I covered this in-depth in a previous article “Testosterone and Fat Loss - the Evidence”.
In “Keep your waist to less than half your height” I introduced the waist-to-height ratio and explained that it is a better tool for predicting health outcomes and mortality than is waist circumference alone. I have also covered the association between a large waist (i.e. belly) and reduced testosterone levels in "Young Men, Waist, Testosterone and Erectile Function: Low-T is not only an old man's issue".
Here I will summarize research showing that the waist-to-height ratio can also be used as a screening tool for testosterone deficiency.
Video Summary: Testosterone Deficiency and Treatment - International Expert Consensus Resolutions
- Published in Testosterone Replacement Therapy

In a previous article "Testosterone Deficiency and Treatment - the FACTS" I presented the conclusions from an International Expert Consensus Conference on Testosterone Deficiency and Its Treatment.[1]
Here I summarize the key points, and link to a video summary by Dr. Abraham Morgentaler, an internationally renowned testosterone scientist and clinician.
Long-term testosterone treatment with different testosterone preparations - provocative results on diagnosis and adherence
- Published in Testosterone Replacement Therapy

Due to lack of consistent clear-cut guidelines for diagnosis and treatment of testosterone deficiency, there is a lot of confusion among both health professionals and suffering men. The multiple different testosterone preparations available further add to the complexity of testosterone treatment.
This article presents the intriguing results from a notable study that analyzed effects of testosterone therapy with seven different testosterone preparations in symptomatic men who had previously been denied treatment because of “normal” baseline testosterone levels.[1]
The results are quite provocative and highlight several important practical issues relating to diagnosis and treatment of hypogonadism…
Is Testosterone Replacement Therapy a Lifelong Treatment?
- Published in Testosterone Replacement Therapy

A common question among hypogonadal men is how long they should stay on testosterone therapy.
The answer is - it depends on what is causing a man’s testosterone deficiency..
Health Consequences of Subclinical Testosterone Deficiency - riskier than previously thought
- Published in Testosterone - Men

In discussions about diagnosis and health consequences of hypogonadism, aka testosterone deficiency, the prime focus is given to testosterone levels and signs/symptoms.[1-3] However, emerging research has identified a less clinically evident gonadal dysfunction called “subclinical” hypogonadism (or “compensated” hypogonadism).[4, 5]
Subclinical hypogonadism is characterized by normal testosterone levels in the presence of elevated LH level. As testosterone levels are not markedly reduced in subclinical hypogonadism, intuitively one may think it does not confer negative health consequences.
However, a recent study by Corona et al., which specifically was conducted to investigate the potential health ramifications of subclinical hypogonadism, shows that it should not be neglected. Surprisingly, subclinical hypogonadism is associated with an almost 10-fold increased risk of cardiovascular mortality, which is comparable to that for overt hypogonadism! [6]
Testosterone Therapy and Cardiovascular Risk - Advances and Controversies
- Published in Testosterone Replacement Therapy
One of the most debated issues related to testosterone therapy is its effects on cardiovascular risk and clinical events, like for example heart attack.
January 27th, 2015 a comprehensive medical review paper was published, addressing the controversial topic of testosterone therapy and cardiovascular risk.[65] It was written by the Androgen Study Group academicians and published in Mayo Clinic Proceedings.
Here I summarizes key conclusions from this milestone medical review.
How well informed are general practitioners and cardiologists about testosterone deficiency and its consequences?
- Published in Testosterone - Men

A rapidly growing body of medical research is showing that testosterone deficiency (aka hypogonadism and low-T) is strongly associated with a wide range of detrimental health outcomes [1, 2], and that testosterone replacement therapy improves those health parameters that are negatively affected by testosterone deficiency.[2, 3]
Therefore, leading testosterone scientists now view testosterone deficiency as a cardiovascular risk factor that contributes to the development of cardiovascular disease.[4-7]
As general practitioners and cardiologists primarily care for these patients with cardiovascular disease, a survey study was conducted to assess their knowledge, beliefs and clinical practice with respect to testosterone deficiency and cardiovascular health.[8]
Testosterone Boosting Medications and Cardiovascular Risk - a systematic review and meta-analysis
- Published in Testosterone Replacement Therapy
Accumulating evidence shows beneficial effect of testosterone therapy on a wide range of health outcomes, including inflammation, insulin sensitivity, muscle mass, body fat mass, lipid profiles, endothelial, bone mineral density, energy and vitality, mood, sexual function and overall quality of life. [1-9]
Despite this, concerns have been raised that testosterone therapy could have detrimental effects on cardiovascular disease.
In this article I summarize results from a comprehensive systematic review and meta-analysis, the largest to date, of all placebo-controlled randomized clinical trials (RCTs) on the effect of testosterone therapy on cardiovascular-related outcomes.[10]
Is hypogonadism, aka "andropause", the male version of menopause?
- Published in Testosterone - Men

Many men who reach middle-age start to experience symptoms that resemble those of menopause; reduced libido, lack of energy, weight gain, fatigue, depression and osteoporosis, to name a few.[1-5]



