Remnant Cholesterol and non-HDL – What’s that? Why bother?

non-HDL-C
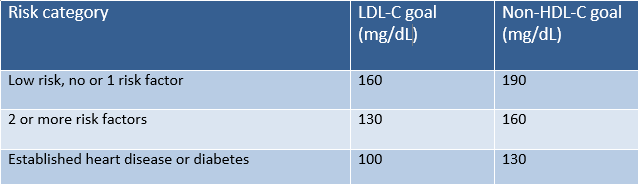
Remnant cholesterol
Summary
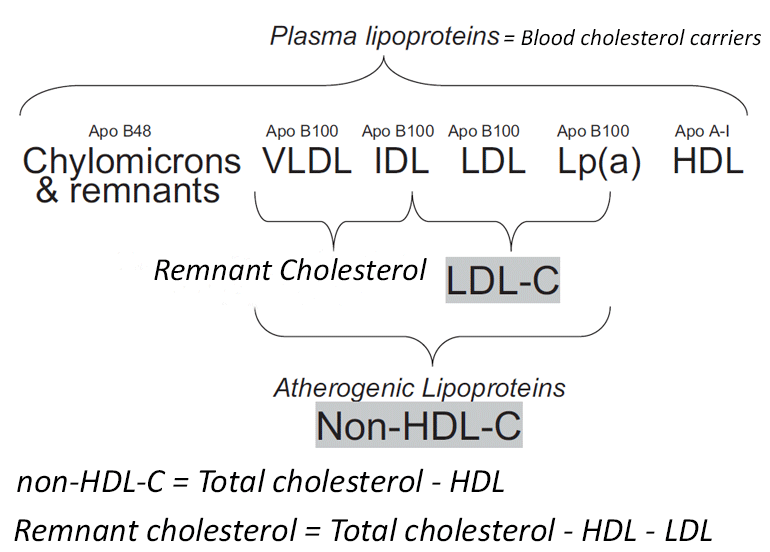
Figure modified from Robinson JG. Are you targeting non-high-density lipoprotein cholesterol? J Am Coll Cardiol. 2009 Dec 29;55(1):42-4.
References:
1. Arsenault, B.J., et al., Beyond low-density lipoprotein cholesterol: respective contributions of non-high-density lipoprotein cholesterol levels, triglycerides, and the total cholesterol/high-density lipoprotein cholesterol ratio to coronary heart disease risk in apparently healthy men and women. J Am Coll Cardiol, 2009. 55(1): p. 35-41.
2. Virani, S.S., et al., Barriers to non-HDL cholesterol goal attainment by providers. Am J Med, 2011. 124(9): p. 876-80 e2.
3. Catapano, A.L., et al., ESC/EAS Guidelines for the management of dyslipidaemias The Task Force for the management of dyslipidaemias of the European Society of Cardiology (ESC) and the European Atherosclerosis Society (EAS). Atherosclerosis, 2011. 217(1): p. 3-46.
4. Bays, H.E., et al., National Lipid Association Annual Summary of Clinical Lipidology 2015. J Clin Lipidol, 2015. 8: p. S1-S36.
5. Bays, H.E., et al., Obesity, adiposity, and dyslipidemia: a consensus statement from the National Lipid Association. J Clin Lipidol, 2013. 7(4): p. 304-83.
6. Arsenault, B.J., S.M. Boekholdt, and J.J. Kastelein, Lipid parameters for measuring risk of cardiovascular disease. Nat Rev Cardiol, 2011. 8(4): p. 197-206.
7. Adiels, M., et al., Overproduction of very low-density lipoproteins is the hallmark of the dyslipidemia in the metabolic syndrome. Arterioscler Thromb Vasc Biol, 2008. 28(7): p. 1225-36.
8. Expert Dyslipidemia Panel of the International Atherosclerosis Society Panel, An International Atherosclerosis Society Position Paper: global recommendations for the management of dyslipidemia--full report. J Clin Lipidol, 2014. 8(1): p. 29-60.
9. Bays, H.E., et al., National Lipid Association Annual Summary of Clinical Lipidology 2016. J Clin Lipidol, 2016. 10(1 Suppl): p. S1-S43.
10. Boekholdt, S.M., et al., Association of LDL cholesterol, non-HDL cholesterol, and apolipoprotein B levels with risk of cardiovascular events among patients treated with statins: a meta-analysis. JAMA, 2012. 307(12): p. 1302-9.
11. Denke, M.A., C.T. Sempos, and S.M. Grundy, Excess body weight. An underrecognized contributor to high blood cholesterol levels in white American men. Arch Intern Med, 1993. 153(9): p. 1093-103.
12. Gardner, C.D., M.A. Winkleby, and S.P. Fortmann, Population frequency distribution of non-high-density lipoprotein cholesterol (Third National Health and Nutrition Examination Survey [NHANES III], 1988-1994). Am J Cardiol, 2000. 86(3): p. 299-304.
13. Wolf, R.N. and S.M. Grundy, Influence of weight reduction on plasma lipoproteins in obese patients. Arteriosclerosis, 1983. 3(2): p. 160-9.
14. Yusuf, S., et al., Obesity and the risk of myocardial infarction in 27,000 participants from 52 countries: a case-control study. Lancet, 2005. 366(9497): p. 1640-9.
15. Liu, J., et al., Non-high-density lipoprotein and very-low-density lipoprotein cholesterol and their risk predictive values in coronary heart disease. Am J Cardiol, 2006. 98(10): p. 1363-8.
16. Pischon, T., et al., Non-high-density lipoprotein cholesterol and apolipoprotein B in the prediction of coronary heart disease in men. Circulation, 2005. 112(22): p. 3375-83.
17. Varbo, A., M. Benn, and B.G. Nordestgaard, Remnant cholesterol as a cause of ischemic heart disease: evidence, definition, measurement, atherogenicity, high risk patients, and present and future treatment. Pharmacol Ther, 2014. 141(3): p. 358-67.
18. Nordestgaard, B.G., Triglyceride-Rich Lipoproteins and Atherosclerotic Cardiovascular Disease: New Insights From Epidemiology, Genetics, and Biology. Circ Res, 2016. 118(4): p. 547-63.
19. Varbo, A., et al., Remnant cholesterol as a causal risk factor for ischemic heart disease. J Am Coll Cardiol, 2013. 61(4): p. 427-36.
20. Varbo, A., J.J. Freiberg, and B.G. Nordestgaard, Extreme nonfasting remnant cholesterol vs extreme LDL cholesterol as contributors to cardiovascular disease and all-cause mortality in 90000 individuals from the general population. Clin Chem, 2015. 61(3): p. 533-43.
21. Langsted, A., et al., Nonfasting cholesterol and triglycerides and association with risk of myocardial infarction and total mortality: the Copenhagen City Heart Study with 31 years of follow-up. J Intern Med, 2011. 270(1): p. 65-75.
22. Faergeman, O., et al., Plasma triglycerides and cardiovascular events in the Treating to New Targets and Incremental Decrease in End-Points through Aggressive Lipid Lowering trials of statins in patients with coronary artery disease. Am J Cardiol, 2009. 104(4): p. 459-63.
23. Miller, M., et al., Impact of triglyceride levels beyond low-density lipoprotein cholesterol after acute coronary syndrome in the PROVE IT-TIMI 22 trial. J Am Coll Cardiol, 2008. 51(7): p. 724-30.



