Survival and cardiovascular events in men on testosterone treatment

Key Points
What is known
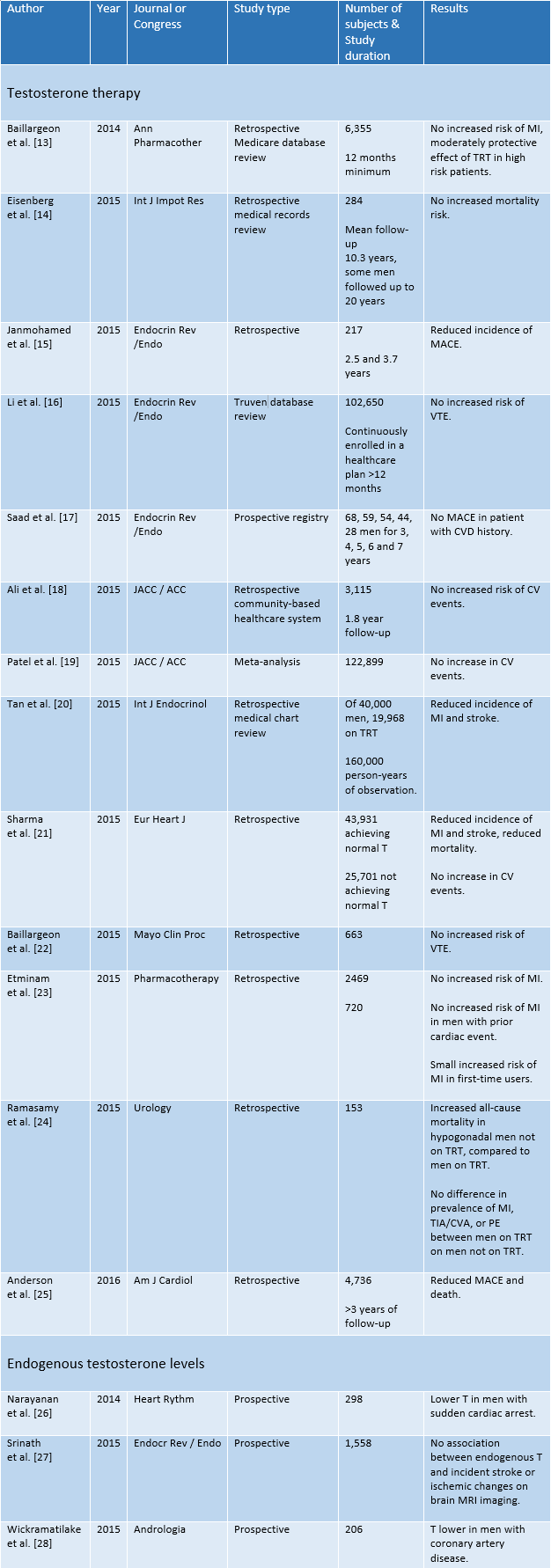
Abbreviations:
T; testosterone, TRT; testosterone replacement therapy, MACE; Major Adverse Cardiovascular Event, VTE; Venous Thromboembolism, TIA; transient ischemic attack, CVA; cerebrovascular accident (aka "stroke"), PE pulmonary embolism; MI, myocardial infarction
What this study adds
Comments
References:
1. Wallis, C.J.D., et al., Survival and cardiovascular events in men treated with testosterone replacement therapy: an intention-to-treat observational cohort study. The Lancet Diabetes & Endocrinology, 2016. May 7.
2. Traish, A.M., Adverse health effects of testosterone deficiency (TD) in men. Steroids, 2014. 88C: p. 106-116.
3. Moeny, D. and J. Staffa. Joint meeting for bone, reproductive and urologic drugs advisory committee (BRUDAC) and the drug safety and risk management advisory committee (DSARM AC): the potential for adverse cardiovascular outcomes associated with use of TRT. US Food and Drug Administration: Sept 17, 2014.
4. Morgentaler, A., Controversies and Advances With Testosterone Therapy: A 40-Year Perspective. Urology, 2016. 89: p. 27-32.
5. Morgentaler, A., et al., Testosterone therapy and cardiovascular risk: advances and controversies. Mayo Clin Proc, 2015. 90(2): p. 224-51.
6. Corona, G., E. Maseroli, and M. Maggi, Injectable testosterone undecanoate for the treatment of hypogonadism. Expert Opin Pharmacother, 2014: p. 1-24.
7. Corona, G., et al., Cardiovascular risk associated with testosterone-boosting medications: a systematic review and meta-analysis. Expert Opin Drug Saf, 2014. 13(10): p. 1327-51.
8. Corona, G.G., et al., Testosterone Replacement Therapy and Cardiovascular Risk: A Review. World J Mens Health, 2015. 33(3): p. 130-42.
9. Ford, E.S., C. Li, and G. Zhao, Prevalence and correlates of metabolic syndrome based on a harmonious definition among adults in the US. J Diabetes, 2010. 2(3): p. 180-93.
10. El Brini, O., et al., Prevalence of metabolic syndrome and its components based on a harmonious definition among adults in Morocco. Diabetes Metab Syndr Obes, 2014. 7: p. 341-6.
11. Botoseneanu, A., et al., Prevalence of metabolic syndrome and its association with physical capacity, disability, and self-rated health in Lifestyle Interventions and Independence for Elders Study participants. J Am Geriatr Soc, 2015. 63(2): p. 222-32.
12. Yang, L. and G.A. Colditz, Prevalence of Overweight and Obesity in the United States, 2007-2012. JAMA Intern Med, 2015. 175(8): p. 1412-3.
13. Baillargeon, J., et al., Risk of Myocardial Infarction in Older Men Receiving Testosterone Therapy. Ann Pharmacother, 2014. 48(9): p. 1138-1144.
14. Eisenberg, M.L., et al., Testosterone therapy and mortality risk. Int J Impot Res, 2015. 27(2): p. 46-8.
15. Janmohamed, S., et al., The Association Between Testosterone Use and Major Adverse Cardiovascular Events (MACE): An Exploratory Retrospective Cohort Analysis of Two Large, Contemporary, Coronary Heart Disease Clinical Trials, in Testosterone Replacement Therapy: Risks and Benefits. 2015. p. OR34-4-OR34-4.
16. Li, H., et al., Assessment of the Association Between the Use of Testosterone Replacement Therapy (TRT) and the Risk of Venous Thrombotic Events Among TRT-Treated and Untreated Hypogonadal Men, in Testosterone Replacement Therapy: Risks and Benefits. 2015. p. OR34-2-OR34-2.
17. Saad, F., et al., Obese Hypogonadal Men with Cardiovascular Diseases (CVD) Benefit from Long-Term Treatment with Testosterone Undecanoate (TU): Observational, Real-Life Data from a Registry Study, in Male Hypogonadism - Causes and Treatments. 2015. p. SAT-135-SAT-135.
18. Ali, Z., et al., Effects of testosterone supplement therapy on cardiovascular outcomes in men with low testosterone. Journal of the American College of Cardiology, 2015. 65(March).
19. Patel, P., et al., Effect of testosterone therapy on adverse cardiovasular events among men: a meta-analysis. Journal of the American College of Cardiology, 2015. 65(March).
20. Tan, R.S., K.R. Cook, and W.G. Reilly, Myocardial Infarction and Stroke Risk in Young Healthy Men Treated with Injectable Testosterone. Int J Endocrinol, 2015. 2015: p. 970750.
21. Sharma, R., et al., Normalization of testosterone level is associated with reduced incidence of myocardial infarction and mortality in men. Eur Heart J, 2015. 36(40): p. 2706-15.
22. Baillargeon, J., et al., Risk of Venous Thromboembolism in Men Receiving Testosterone Therapy. Mayo Clin Proc, 2015. 90(8): p. 1038-45.
23. Etminan, M., et al., Testosterone therapy and risk of myocardial infarction: a pharmacoepidemiologic study. Pharmacotherapy, 2015. 35(1): p. 72-8.
24. Ramasamy, R., et al., Association Between Testosterone Supplementation Therapy and Thrombotic Events in Elderly Men. Urology, 2015. 86(2): p. 283-5.
25. Anderson, J.L., et al., Impact of Testosterone Replacement Therapy on Myocardial Infarction, Stroke, and Death in Men With Low Testosterone Concentrations in an Integrated Health Care System. Am J Cardiol, 2016. 117(5): p. 794-9.
26. Narayanan, K., et al., Sex hormone levels in patients with sudden cardiac arrest. Heart Rhythm, 2014. 11(12): p. 2267-72.
27. Srinath, R., et al., Association Between Endogenous Testosterone and Incident Stroke and Ischemic Changes on Brain MRI in Men in the Atherosclerosis Risk in Communities (ARIC) Cohort, in Testosterone Replacement Therapy: Risks and Benefits. 2015. p. OR34-3-OR34-3.
28. Wickramatilake, C.M., et al., Testosterone and high-sensitive C-reactive protein in coronary artery disease patients awaiting coronary artery bypass graft. Andrologia, 2015. 47(5): p. 493-8.
29. Saad, F., et al., Onset of effects of testosterone treatment and time span until maximum effects are achieved. Eur J Endocrinol, 2011. 165(5): p. 675-85.
30. Traish, A.M., et al., The dark side of testosterone deficiency: I. Metabolic syndrome and erectile dysfunction. J Androl, 2009. 30(1): p. 10-22.
31. Traish, A.M., F. Saad, and A. Guay, The dark side of testosterone deficiency: II. Type 2 diabetes and insulin resistance. J Androl, 2009. 30(1): p. 23-32.
32. Traish, A.M., et al., The dark side of testosterone deficiency: III. Cardiovascular disease. J Androl, 2009. 30(5): p. 477-9



