Effects of Testosterone Therapy for 3 Years on Subclinical Atherosclerosis Progression in Older Men
- Published in Testosterone Replacement Therapy
- Written by Monica
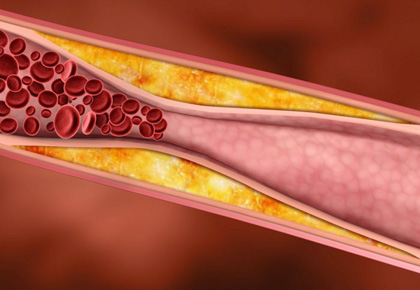
Clinical practice guidelines rely heavily on results from randomized controlled trials (RCTs), which is the gold standard for medical research. RCTs produce evidence considered to be of the highest quality. Because RCTs are resource intensive and costly, they are typically of relatively short duration, commonly lasting for around one year.
Currently there are only a few placebo-controlled RCTs investigating the effects of testosterone therapy for a duration of 3 years [1-4], and medical societies have long been urging for more long-term trials evaluating the safety and efficacy of testosterone therapy.[5-7]
On August 11th 2015 a notable 3-year long RCT was published in JAMA (Journal of the American Medical Association), which attracted a lot of attention.[8] While interpreted by many as showing that testosterone therapy does not confer any benefits on atherosclerosis, sexual function and quality of life, a closer look at the data actually shows two important positive results…
Article Tags
Normalization of testosterone level is associated with reduced risk of heart attack, stroke and mortality in men
- Published in Testosterone Replacement Therapy
- Written by Monica
The effect of testosterone replacement therapy on cardiovascular outcomes such as heart attack and stroke are controversial and have been generating heated discussions among clinicians as well as researchers. This, coupled with biased media sensationalism blowing up the supposed “dangers” of testosterone therapy has created great confusion among suffering men, who could gain tremendous health benefits from testosterone therapy.[1]
Here I report the results of a new study that examined the relationship between normalization of total testosterone levels with testosterone therapy and cardiovascular events as well as all-cause mortality, in patients without a previous history of heart attack and stroke.[2] This notable study was published in the European Heart Journal on August 6th, 2015.
Article Tags
Niacin – a.k.a vitamin B3 – the neglected broad spectrum cholesterol drug!
- Published in Diet, Nutrition & Supplements
- Written by Monica
Niacin - vitamin B3 - when taken in high dose acts as a powerful cholesterol drug. Niacin is unique among all available cholesterol drugs because it has beneficial effects across the entire lipid/lipoprotein spectrum, including the three components of atherogenic dyslipidemia.
Article Tags
Long-term testosterone treatment with different testosterone preparations - provocative results on diagnosis and adherence
- Published in Testosterone Replacement Therapy
- Written by Monica

Due to lack of consistent clear-cut guidelines for diagnosis and treatment of testosterone deficiency, there is a lot of confusion among both health professionals and suffering men. The multiple different testosterone preparations available further add to the complexity of testosterone treatment.
This article presents the intriguing results from a notable study that analyzed effects of testosterone therapy with seven different testosterone preparations in symptomatic men who had previously been denied treatment because of “normal” baseline testosterone levels.[1]
The results are quite provocative and highlight several important practical issues relating to diagnosis and treatment of hypogonadism…
Article Tags
Risk of Blood Clots in Men Receiving Testosterone Therapy?
- Published in Testosterone Replacement Therapy
- Written by Monica
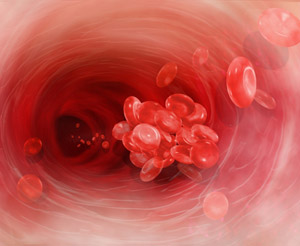
Venous thromboembolism is a blood clot that forms in a vein deep inside a part of the body; it mainly affects the large veins in the lower leg and thigh.
Blood clot formation (venous thromboembolism) has been suggested to be one main risk with testosterone replacement therapy. In 2014, both the US Food and Drug Administration (FDA) [1] and Health Canada [2] implemented a requirement for manufacturers to add a warning about the potential risks of venous thromboembolism and deep vein thrombosis to the label of all testosterone products.
However, until recently there were no comparative studies examining an association between testosterone replacement therapy and venous thromboembolism. Here we report the results of a recent case-control study - published July 20th 2015 - that specifically examined the risk of venous thromboembolism associated with testosterone therapy in middle-aged and older men.[3]
Article Tags
Artificial Sweeteners and Diet Sodas - do they Help or Hinder Fat Loss?
- Published in Diet, Nutrition & Supplements
- Written by Monica

The potential benefits and risks of artificial sweeteners and diet sodas are hotly debated. Critics state that artificial sweeteners and diet sodas are fueling obesity [1, 2], increasing the risk for diabetes and cardiovascular disease [2, 3], and of causing metabolic derangements.[2]
A popular argument against consumption of sweet-tasting but non-caloric or reduced-calorie food and beverages is that this interferes with appetite and physiological energy intake regulation.[2]
Article Tags
Why you need to look beyond your LDL - “bad cholesterol” - level
- Published in Cardiovascular Disease
- Written by Monica

In the United States, cardiovascular diseases account for about 1 of every 3 deaths.[1] The cornerstone in heart disease treatment is reducing elevations of LDL, popularly known as the “bad cholesterol” (see table below “What do the terms mean?”) [2, 3], primarily with statins, the most widely used cholesterol/ heart disease drug.[4]
However, when one looks at the aggregate effectiveness of statin treatment in all studies, morbidity and mortality rates among statin-treated patients still remain approximately two thirds to three quarters of those found in patients randomized to placebo.[5, 6] In the “Treating to New Targets” study there were still 80% cases of cardiovascular disease, despite intensive treatment with high-dose statins.[7]
Thus, many patients – even those treated aggressively with statins to meet LDL goals - have residual cardiovascular risk.[8-13] This remaining risk is associated with low levels of HDL, increased levels of triglycerides, and elevated numbers of small, dense, atherogenic LDL particles.[8, 10, 11, 14-17] and other common metabolic abnormalities that you will find out about in this article...
Article Tags
Fish Oil for Fat Loss - can it really help you get in shape?
- Published in Diet, Nutrition & Supplements
- Written by Monica

Fish oil is most known for its beneficial heart and cardiovascular effects, and continues to top the list of health promoting supplements. Fish oil is unique in its ability to protect against heart disease and promote cardiovascular health in all people, regardless of age or baseline health status [1, 2].
Fish oil improves the blood lipid profile and is especially effective at lowering triglycerides (a.k.a. blood fats).[3] It also has beneficial effects on blood platelet activity, blood thickness, as well as blood vessel (endothelial) function [4-11], blood vessel elasticity [12], and blood pressure [13, 14], among other things.
In 2004 FDA approved a prescription fish oil preparation for treatment of high triglycerides (hypertriglyceridemia) [3, 15, 16]. Accumulating research shows that fish oil also has other beneficial effects, which are more visually notable… notably, fat loss!
Article Tags
Aspirin – can it save you from heart disease or cancer?
- Published in Primary Prevention & Lifestyle
- Written by Monica

In people with pre-existing cardiovascular disease, it has long been well documented that long-term use of aspirin is an effective anti-platelet treatment that significantly reduces the risk of serious cardiovascular events (such as heart attacks and strokes) by 30% and cardiovascular death by 15%.[1, 2]
This benefit greatly exceeds the potential risk of increased bleeding events, which is a side effect of aspirin.[3] Therefore clinical guidelines recommend that people with cardiovascular disease take low dose aspirin (75 to 162 mg) daily to prevent recurrence of cardiovascular events.[4-6]
More recently, the use of aspirin in healthy people for prevention of cardiovascular disease, as well as cancer, has been getting more and more attention. However, research on prophylactic use of aspirin conflicting and clinical guidelines are contradictory. Here I will shed some light on new research to help you make an informed decision whether aspirin may protect you…
Article Tags
Red Meat - Good or Bad for Fat Loss?
- Published in Diet, Nutrition & Supplements
- Written by Monica
Consumption of red meat has been associated with fat gain (weight gain) because of its high fat and calorie content. Even though the old idea that “a high fat intake causes body fat gain” has been completely debunked in medical research [1-9], red meat still is a food that's on the forbidden or avoid list in most diet plans. And for some reason, women tend to be especially afraid of eating meat…
While there are studies showing an association between meat intake and obesity [10-12], there are also studies not showing this [12-14]. And when digging deeper in the data, many of the studies that did report a significant association with meat intake and fat gain / obesity have several flaws that invalidate their conclusions....
Article Tags
More...
- Provocative New Research on Testosterone, Prostate Cancer and BPH/LUTS
- Vitamin D - what's the optimal blood level and how to achieve it?
- Nitrate supplementation – ramp up the less well-known NO pathway to boost performance and health
- Testosterone Treatment and Hormonophobia – Cardiovascular risk, the Media, and the Authorities



