6 Best Foods to Help Increase Low Testosterone
- Published in Testosterone Replacement Therapy

Having adequate levels of testosterone is a vital factor in determining your quality of life. For beginners, testosterone is a male sex hormone found in men and women found to be important for energy, fertility, healthy sexual functions, and building muscle. Testosterone is one of the main causes of physical changes for boys during puberty, like promoting deeper voice and hair growth. Generally, a person’s testosterone level will steadily decline as you age, depending on medical conditions, lifestyle choices, and other factors. A decreasing T level can result in a lot of changes in your body, including a lower sex drive.
5 Signs Your Testosterone is Too Low
- Published in Testosterone Replacement Therapy

Like all hormones, testosterone plays an important role in regulating a host of different processes in the body. There is no question maintaining optimal levels of testosterone is ideal to a healthy lifestyle. Testosterone is an essential hormone responsible for male development, masculine characteristics, building muscle, fueling sex drive, and receptors exists throughout the body. This hormone is primarily produced in the male testicles and womens’ adrenal glands. As we age, testosterone production begins to slow down. If you have low levels of testosterone, the consequences can greatly affect your health.
5 Ways to Naturally Boost Your Testosterone
- Published in Testosterone Replacement Therapy

When you see the term “testosterone,” we typically associate it with masculinity and men. However, women generate testosterone too. So, what exactly is testosterone? Testosterone is a steroid hormone that plays a significant role in the male sperm production and produced in women’s ovaries in much smaller amounts. Rising levels of testosterone stimulates physical and chemical changes for boys and men such as increased muscle, pubic hair growth, deeper lengthened vocal chords, and increased sexual desire.
Testosterone production significantly spikes during puberty and starts to drop after age 30. Having optimal levels of the steroid hormone is essential from puberty throughout adulthood for general health, aids in preventing certain chronic diseases, and increases energy levels. As our levels of testosterone naturally decrease over time, rest assured there are ways to naturally boost it back up.
Testosterone treatment is NOT associated with risk of adverse cardiovascular events – the RHYME study
- Published in Testosterone Replacement Therapy
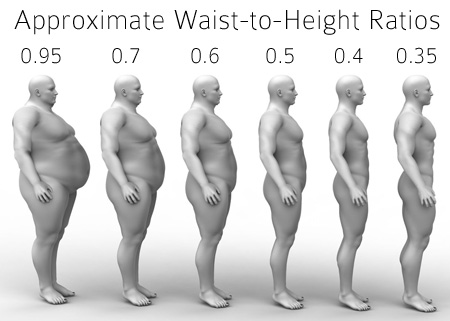
Waist-to-Height Ratio as a Screening Tool for Testosterone Deficiency
- Published in Testosterone Replacement Therapy
Video Summary: Testosterone Deficiency and Treatment - International Expert Consensus Resolutions
- Published in Testosterone Replacement Therapy

Testosterone Deficiency and Treatment - the FACTS
- Published in Testosterone Replacement Therapy

Everything We Learned About TESTOSTERONE Is WRONG - video presentation by Dr. Morgentaler
- Published in Testosterone Replacement Therapy

Long-term testosterone treatment with different testosterone preparations - provocative results on diagnosis and adherence
- Published in Testosterone Replacement Therapy

Due to lack of consistent clear-cut guidelines for diagnosis and treatment of testosterone deficiency, there is a lot of confusion among both health professionals and suffering men. The multiple different testosterone preparations available further add to the complexity of testosterone treatment.
Is Testosterone Replacement Therapy a Lifelong Treatment?
- Published in Testosterone Replacement Therapy




