Testosterone Replacement Therapy
Video Summary of Testosterone Replacement Therapy and Cardiovascular Risk
- Published in Testosterone Replacement Therapy
- Written by Monica

One of the most controversial and debated issue related to testosterone replacement therapy is its effects on cardiovascular risk and related clinical outcomes.
In the February 2015 issue of Mayo Clinic Proceedings a comprehensive medical review paper, written by Dr. Abraham Morgentaler and his coauthors of the Androgen Study Group – www.AndrogenStudyGroup.org - was published.[1]
The aim of the review was to analyze all available studies on testosterone replacement therapy and cardiovascular effects, and to clarify the grossly misleading conclusions from two recent studies that caused a tremendous media scare.
In this 8 minute video, Dr. Morgentaler presents the key results from this comprehensive analysis…
Article Tags
Is Testosterone Replacement Therapy a Lifelong Treatment?
- Published in Testosterone Replacement Therapy
- Written by Monica

A common question among hypogonadal men is how long they should stay on testosterone therapy.
The answer is - it depends on what is causing a man’s testosterone deficiency..
Article Tags
Testosterone Therapy and Cardiovascular Risk - Advances and Controversies
- Published in Testosterone Replacement Therapy
- Written by Monica
One of the most debated issues related to testosterone therapy is its effects on cardiovascular risk and clinical events, like for example heart attack.
January 27th, 2015 a comprehensive medical review paper was published, addressing the controversial topic of testosterone therapy and cardiovascular risk.[65] It was written by the Androgen Study Group academicians and published in Mayo Clinic Proceedings.
Here I summarizes key conclusions from this milestone medical review.
Article Tags
Testosterone, Mortality and Longevity
- Published in Testosterone Replacement Therapy
- Written by Monica

Population studies show that men with low or low-normal testosterone levels are at an increased risk of mortality compared to those with higher levels, and that cardiovascular disease accounts for the greater proportion of deaths in men with low testosterone.[1]
Here I summarize a medical review paper which addressed the following two questions: [1]
1. Is testosterone deficiency directly involved in the pathogenesis of these conditions or is it merely a biomarker of ill health and the severity of underlying disease processes?
2. Does testosterone replacement therapy retard disease progression and ultimately enhance the clinical prognosis and survival?
Article Tags
Testing for testosterone deficiency - things to know about the blood draw
- Published in Testosterone Replacement Therapy
- Written by Monica
The first step (aside from identifying symptoms) in diagnosing testosterone deficiency, aka low-T, is to do a blood test.
Here I cover some important practical things to know about a blood draw for testosterone analysis...
Article Tags
Cardiovascular Risks and Elevations of Blood DHT Levels Vary by Testosterone Preparation
- Published in Testosterone Replacement Therapy
- Written by Monica
The cardiovascular effects of testosterone and testosterone therapy are subject to intense investigation in medical research and have recently generated heated discussions among healthcare professionals.
While the main focus has been on testosterone per se, it is important to remember that testosterone is both a hormone in its own right, and a pro-hormone that gets converted to both estradiol and DHT (dihydrotestosterone). Estradiol and DHT exert effects themselves that are different from the effects of testosterone.
Therefore, when analyzing the effects of testosterone, especially supplemental testosterone administered as testosterone replacement therapy, it is critical to take into consideration how it affects downstream testosterone metabolites like estradiol and DHT.
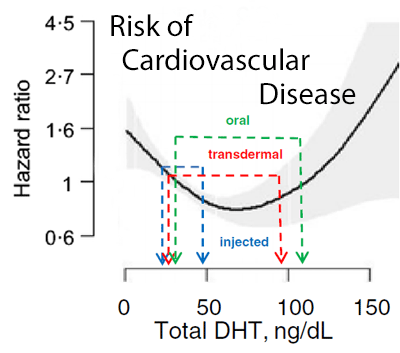
Here I will present results from a recent systematic review and meta-analysis that specifically investigated how different routes of testosterone therapy administration (i.e different testosterone preparations) affect blood levels of testosterone and espcially DHT , and how this in turn relates to cardiovascular adverse events.[1]
Article Tags
Testosterone and Fat Loss - the Evidence
- Published in Testosterone Replacement Therapy
- Written by Monica

It is well documented that obesity may cause hypogonadism, and that hypogonadism may cause obesity [1-4] This has generated debate about what condition comes first; obesity or hypogonadism? And what should be the first point of intervention?
In this article I will summarize data from several reviews on the associations of hypogonadism and obesity [1-4], and make the case that these conditions create a self-perpetuating vicious circle. Once a vicious circle has been established, it doesn’t matter where one intervenes; one can either treat the obese condition or treat hypogonadism first. The critical issue is to break the vicious circle as soon as possible before irreversible health damage arises.
Nevertheless, as I will explain here, treating hypogonadism first with testosterone replacement therapy may prove to be a more effective strategy because it to a large extent “automatically” takes care of the excess body fat and metabolic derangements. In addition, treating hypogonadism first also confers psychological benefits that will help obese men become and stay more physically active.
Article Tags
Testosterone Therapy Prevents Gain in Intra-Abdominal Fat and Counteracts Loss of Muscle in Non-Obese Aging Men
- Published in Testosterone Replacement Therapy
- Written by Monica

Testosterone deficiency is especially common in men who are obese and/or have the metabolic syndrome or diabetes, with a prevalence ranging from 35% to almost 80%.[1-5] However, there is a subgroup of non-obese men who have low testosterone levels and suffer from typical symptoms of low-T, but who do not (yet) have any co-morbidities.
Many studies show that suboptimal testosterone levels may contribute to the development of obesity (including abdominal obesity) [6, 7], metabolic syndrome [8-13] and/or diabetes.[9, 14-20] Therefore, testosterone therapy in non-obese men with testosterone deficiency may be an effective intervention to correct not only symptoms associated with hypogonadism, but also prevent the development of obesity, metabolic syndrome and/or diabetes.
A notable study was set out to specifically investigate this…
Article Tags
Estrogen elevations in response to Testosterone Therapy – to treat or not?
- Published in Testosterone Replacement Therapy
- Written by Monica

During testosterone therapy, total and free estradiol (the main form of estrogen) levels increase dose-dependently in both young (aged 19-35 year old) and 52 older (aged 59-75 year old) men, and more so in older men compared to younger men.[1]
The potential clinical consequences of higher estradiol levels and higher estradiol-to-testosterone ratios in older men remains poorly understood, and the optimal management of high-normal or elevated estrogens is controversial among clinicians.[2]
Interestingly, in some patients, an initial elevation in estradiol is followed by decreased estradiol after prolonged testosterone therapy.[3, 4] This may be due to reduced body fat mass or decreased testosterone levels over time with fixed dose treatments.
Here you will get advice on how to best approach estrogen management while on testosterone therapy…
Article Tags
Testosterone Boosting Medications and Cardiovascular Risk - a systematic review and meta-analysis
- Published in Testosterone Replacement Therapy
- Written by Monica
Accumulating evidence shows beneficial effect of testosterone therapy on a wide range of health outcomes, including inflammation, insulin sensitivity, muscle mass, body fat mass, lipid profiles, endothelial, bone mineral density, energy and vitality, mood, sexual function and overall quality of life. [1-9]
Despite this, concerns have been raised that testosterone therapy could have detrimental effects on cardiovascular disease.
In this article I summarize results from a comprehensive systematic review and meta-analysis, the largest to date, of all placebo-controlled randomized clinical trials (RCTs) on the effect of testosterone therapy on cardiovascular-related outcomes.[10]
Article Tags
More...
- Incidence of Prostate Cancer after Testosterone Therapy for up to 17 years
- Adherence to testosterone therapy - short term treatment is not sufficient for achievement of maximal benefits
- Efficacy and safety of injectable testosterone undecanoate (Aveed or Nebido) for the treatment of hypogonadism
- Testosterone Levels, Testosterone Therapy and Cardiovascular Risk in Men



