Testosterone deficiency is especially common in men who are obese and/or have the metabolic syndrome or diabetes, with a prevalence ranging from 35% to almost 80%.[1-5] However, there is a subgroup of non-obese men who have low testosterone levels and suffer from typical symptoms of low-T, but who do not (yet) have any co-morbidities.
Many studies show that suboptimal testosterone levels may contribute to the development of obesity (including abdominal obesity) [6, 7], metabolic syndrome [8-13] and/or diabetes.[9, 14-20] Therefore, testosterone therapy in non-obese men with testosterone deficiency may be an effective intervention to correct not only symptoms associated with hypogonadism, but also prevent the development of obesity, metabolic syndrome and/or diabetes.
60 healthy but symptomatic, non-obese men aged 55 years or older with total testosterone levels less than 433 ng/dL (15 nmol/L) were randomized to transdermal testosterone or placebo for 52 weeks.
Subjects were instructed not to significantly modify their dietary or exercise patterns during the study.
Hormone levels, metabolic parameters and the following body composition parameters were measured at week 0 and 52:
Fat mass, fat free mass and muscle mass (measured by DEXA).
Abdominal subcutaneous and intra-abdominal (visceral) adipose tissue, thigh muscle, and inter-muscular fat (measured MRI).
RESULTS:
In the testosterone group, total testosterone levels significantly increased by 30% (115 ng/dL), from a baseline mean level of 392 ng/dL to 505 ng/dL.
Free testosterone levels significantly increased by 40% (43 pg/mL), from a baseline mean 107 pg/mL to 150 pg/mL.
In the placebo group, total testosterone levels fell by 10% while there was no change in free testosterone levels.
SHBG (sex hormone binding globulin) and estradiol levels did not change significantly in either group.
Fat free mass tended to increase in the testosterone group and was unchanged in the placebo group. The gain in fat free mass was confined to the appendices with an increase in leg and arm fat free mass in the testosterone group relative to placebo.
In line with the increase in fat free mass relative to placebo, thigh and (to a lesser extent) arm muscle mass tended to increase in the testosterone group, while a significant 4.1% decrease in thigh muscle mass was observed in the placebo group. This led to a significant difference between the groups in muscle mass at the end of the 1 year-long study.
While there was no change in total body fat mass or abdominal subcutaneous fat mass, intra-abdominal fat mass was reduced in the testosterone group and increased in the placebo groups, such that there was a significant difference between the groups at the end of the 1 year-long study.
The change in intra-abdominal fat was correlated significantly with the change in total testosterone levels; men with the greatest increases in testosterone levels had the greatest reductions in intra-abdominal fat.
The testosterone group also had a significant reduction in thigh subcutaneous fat mass.
Testosterone treatment did not affect neither LDL, HDL, triglycerides (aka blood fats), fasting blood glucose levels, fasting insulin nor insulin resistance. However, the placebo group showed a significant 10% increase in total and LDL cholesterol.
Hemoglobin levels significantly increased in the testosterone group from (15.2 to 15.6 g/dL), but not in the placebo group.
Hematocrit did not change in either group.
No abnormalities in digital rectal examination were recorded.
Testosterone treatment did not affect PSA levels, which were 2.1 g/L at the start and end of the study.
CONCLUSION:
Testosterone therapy, relative to placebo, selectively reduces visceral fat accumulation without change in total body fat mass, and increases total body fat free mass and total body and thigh muscle mass.
Comments
This study raises several important points:
Baseline testosterone levels and “thresholds” for hypogonadism diagnosis
Middle age men with symptoms of testosterone deficiency benefit from testosterone replacement therapy even when their baseline testosterone levels are higher than the suggested hypogonadal thresholds of 300 ng/dL (US Endocrine Society)[22] or 350 ng/dL (European Association of Urology).[23] This is important to underscore, as many doctors will deny testosterone treatment to men whose testosterone level is above these thresholds.
Regarding the so called “thresholds” for hypogonadism diagnosis, it should be borne in mind that they are arbitrarily set. There is no one-single testosterone level that is optimal for every man. This is why it is important for men to consult with a doctor who is well versed in men’s health and knows how to look at the whole clinical picture.
This study also shows that even relatively small increases in testosterone levels confer benefits in terms of body composition, especially on intra-abdominal fat mass and muscle mass.
Fat mass and fat distribution
In this study no effect of testosterone therapy was seen on total body fat mass. This is in contrast to the 5–15% (up to 4.5 kg) decrease at 12 months in other studies which achieved larger increases in total testosterone levels, up to 744 ng/dL.[24-28] Therefore, the lack of effect on fat mass in this current study may be due to the more modest rise in total testosterone levels (505 ng/dL). It could also be due to the subjects’ lower baseline fat mass and/or higher baseline testosterone levels.
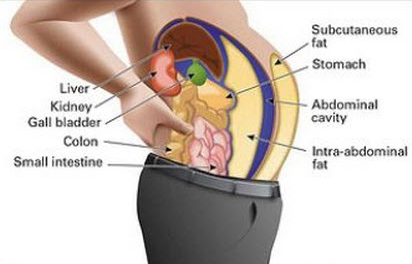
However, the study reported here did show that testosterone therapy in non-obese men prevents accumulation of intra-abdominal fat compared to placebo.[21] Thus, even relatively modest increases in testosterone levels effectively targets loss of intra-abdominal fat mass, with the reduction in intra-abdominal fat mass being greater with greater increases in testosterone levels. This is consistent with results from other studies of testosterone supplementation in eugonadal (non-hypogonadal) middle-aged abdominally obese men (mean BMI 29 and waist circumference 41 inches = 105 cm) in which decreases in intra-abdominal fat mass of 5-10% (0.9 to 1.3 lb) were shown after 8-9 months.[29, 30]
Intra-abdominal fat mass is the body fat depot that preferentially increases with advancing age [31-33] and is one of the major risk factors of aging related chronic diseases, including type 2 diabetes, high blood pressure, cardiovascular diseases, and cancers, and, ultimately, death.[33-35] Intra-abdominal fat is a strong, independent predictor of all-cause mortality in men.[36] As men have larger intra-abdominal fat depots than women [37], it possibly contributes to men’s shorter life expectancy. It has actually been proposed that targeting reduction in intra-abdominal fat mass could be a potential treatment strategy to prevent or delay age-related diseases and to increase longevity.[38]
Therefore, one may argue that testosterone therapy in men with sub-optimal testosterone levels (even if they are higher than proposed hypogonadism thresholds) may serve as a preventive strategy against future accumulation of intra-abdominal fat and its consequences.
Fat free mass and muscle mass
The trend for progressive loss of fat free mass in placebo group (presumably reflecting an aging effect) combined with the upward trend in the testosterone-treated men led to significant group difference at the end of the 1 year-long study. [21] The loss of fat free mass in the placebo group is consistent with the 0.9 lb loss of fat free mass per year seen in men beyond their fifth decade.[39]

The significant 4% loss of thigh muscle over 12 months in the placebo group, and the trend to an increase in the testosterone group, indicates that elevation of testosterone levels from the low-normal range into the mid-normal range may ameliorate age-related sarcopenia. Similar effects on muscle mass have been reported in studies of apparently healthy men aged 19 to 75 years, who were rendered hypogonadal (with a GnRH agonist) and then given testosterone therapy to return testosterone levels to different target ranges.[7, 40] Sub-physiological testosterone doses resulted in loss of muscle while supra-physiological doses led to clear gains of muscle mass.
The finding that testosterone therapy prevented loss of thigh skeletal muscle is notable because as men age they lose muscle mass more rapidly than other components of the fat free mass [41], and because there is relatively greater loss of muscle in the lower body compared with the upper body.[42]
Conclusion
This study clearly shows that the arbitrarily set thresholds for diagnosis of hypogonadism are flawed, as men with baseline testosterone levels above 350 ng/dL clearly benefit from testosterone therapy.[21] The finding that testosterone therapy prevents gain in intra-abdominal fat and counteracts loss of muscle mass (primarily leg muscle mass) in non-obese aging men has important implications for primary prevention of obesity, metabolic syndrome, sarcopenia and its complications.

Previous studies have shown that lower baseline testosterone levels independently predict an increase in inta-abdominal fat after 7.5 years of follow-up [6] and loss of muscle mass.[43] Also, decreased muscle mass and increased fat accumulation around the waist (which in large part reflects intra-abdominal fat) are independently related to mortality in older men.[44] Men with low waist circumference (below 40 inches) and above-average muscle mass have the lowest mortality risk.[44]
Therefore, the argument can be made that every man should get his testosterone levels checked, especially if he is feeling symptoms of sexual dysfunction, fatigue, lack of energy/vigor, loss of muscle and strength, and feelings as if “having past one’s peak” etc. Physiological testosterone therapy is safe for the vast majority of men. Ignoring sub-optimal testosterone levels, even if they are above the clinical hypogonadism threshold of 350 ng/dL, may accelerate negative changes in body composition that will ultimately predispose to aging related diseases like metabolic syndrome, cardiovascular disease, diabetes and sarcopenia, and reduce healthy life expectancy.
Correction of sub-optimal testosterone levels, even in apparently healthy men who are not obese, may prove to the best primary prevention strategy for men to ensure a healthy long vigorous life!
References:
1. Caldas, A.D., et al., Relationship between insulin and hypogonadism in men with metabolic syndrome. Arq Bras Endocrinol Metabol, 2009. 53(8): p. 1005-11.
2. Laaksonen, D.E., et al., The metabolic syndrome and smoking in relation to hypogonadism in middle-aged men: a prospective cohort study. J Clin Endocrinol Metab, 2005. 90(2): p. 712-9.
3. Singh, S.K., R. Goyal, and D.D. Pratyush, Is hypoandrogenemia a component of metabolic syndrome in males? Exp Clin Endocrinol Diabetes, 2011. 119(1): p. 30-5.
4. Pellitero, S., et al., Hypogonadotropic hypogonadism in morbidly obese males is reversed after bariatric surgery. Obes Surg, 2012. 22(12): p. 1835-42.
5. Biswas, M., et al., Total and free testosterone concentrations are strongly influenced by age and central obesity in men with type 1 and type 2 diabetes but correlate weakly with symptoms of androgen deficiency and diabetes-related quality of life. Clin Endocrinol (Oxf), 2012. 76(5): p. 665-73.
6. Tsai, E.C., et al., Low serum testosterone level as a predictor of increased visceral fat in Japanese-American men. Int J Obes Relat Metab Disord, 2000. 24(4): p. 485-91.
7. Finkelstein, J.S., et al., Gonadal steroids and body composition, strength, and sexual function in men. N Engl J Med, 2013. 369(11): p. 1011-22.
8. Haring, R., et al., Prediction of metabolic syndrome by low serum testosterone levels in men: results from the study of health in Pomerania. Diabetes, 2009. 58(9): p. 2027-31.
9. Laaksonen, D.E., et al., Testosterone and sex hormone-binding globulin predict the metabolic syndrome and diabetes in middle-aged men. Diabetes Care, 2004. 27(5): p. 1036-41.
10. Rodriguez, A., et al., Aging, androgens, and the metabolic syndrome in a longitudinal study of aging. J Clin Endocrinol Metab, 2007. 92(9): p. 3568-72.
11. Tsujimura, A., et al., Is low testosterone concentration a risk factor for metabolic syndrome in healthy middle-aged men? Urology, 2013. 82(4): p. 814-9.
12. Haring, R., et al., The role of sex hormone-binding globulin and testosterone in the risk of incident metabolic syndrome. Eur J Prev Cardiol, 2013. 20(6): p. 1061-8.
13. Brand, J.S., et al., Testosterone, sex hormone-binding globulin and the metabolic syndrome in men: an individual participant data meta-analysis of observational studies. PLoS One, 2014. 9(7): p. e100409.
14. Oh, J.Y., et al., Endogenous sex hormones and the development of type 2 diabetes in older men and women: the Rancho Bernardo study. Diabetes Care, 2002. 25(1): p. 55-60.
15. Haffner, S.M., et al., Low levels of sex hormone-binding globulin and testosterone predict the development of non-insulin-dependent diabetes mellitus in men. MRFIT Research Group. Multiple Risk Factor Intervention Trial. Am J Epidemiol, 1996. 143(9): p. 889-97.
16. Vikan, T., et al., Low testosterone and sex hormone-binding globulin levels and high estradiol levels are independent predictors of type 2 diabetes in men. Eur J Endocrinol, 2010. 162(4): p. 747-54.
17. Lakshman, K.M., S. Bhasin, and A.B. Araujo, Sex hormone-binding globulin as an independent predictor of incident type 2 diabetes mellitus in men. J Gerontol A Biol Sci Med Sci, 2010. 65(5): p. 503-9.
18. Stellato, R.K., et al., Testosterone, sex hormone-binding globulin, and the development of type 2 diabetes in middle-aged men: prospective results from the Massachusetts male aging study. Diabetes Care, 2000. 23(4): p. 490-4.
19. Ding, E.L., et al., Sex differences of endogenous sex hormones and risk of type 2 diabetes: a systematic review and meta-analysis. JAMA, 2006. 295(11): p. 1288-99.
20. Selvin, E., et al., Androgens and diabetes in men: results from the Third National Health and Nutrition Examination Survey (NHANES III). Diabetes Care, 2007. 30(2): p. 234-8.
21. Allan, C.A., et al., Testosterone therapy prevents gain in visceral adipose tissue and loss of skeletal muscle in nonobese aging men. J Clin Endocrinol Metab, 2008. 93(1): p. 139-46.
22. Bhasin, S., et al., Testosterone therapy in men with androgen deficiency syndromes: an Endocrine Society clinical practice guideline. J Clin Endocrinol Metab, 2010. 95(6): p. 2536-59.
23. Dohle, G.R., et al., EAU Guidelines on Male Hypogonadism. 2012, European Association of Urology
24. Page, S.T., et al., Exogenous testosterone (T) alone or with finasteride increases physical performance, grip strength, and lean body mass in older men with low serum T. J Clin Endocrinol Metab, 2005. 90(3): p. 1502-10.
25. Snyder, P.J., et al., Effect of testosterone treatment on body composition and muscle strength in men over 65 years of age. J Clin Endocrinol Metab, 1999. 84(8): p. 2647-53.
26. Kenny, A.M., et al., Effects of transdermal testosterone on bone and muscle in older men with low bioavailable testosterone levels. J Gerontol A Biol Sci Med Sci, 2001. 56(5): p. M266-72.
27. Wittert, G.A., et al., Oral testosterone supplementation increases muscle and decreases fat mass in healthy elderly males with low-normal gonadal status. J Gerontol A Biol Sci Med Sci, 2003. 58(7): p. 618-25.
28. Wang, C., et al., Transdermal testosterone gel improves sexual function, mood, muscle strength, and body composition parameters in hypogonadal men. J Clin Endocrinol Metab, 2000. 85(8): p. 2839-53.
29. Marin, P., et al., Androgen treatment of abdominally obese men. Obes Res, 1993. 1(4): p. 245-51.
30. Marin, P., et al., The effects of testosterone treatment on body composition and metabolism in middle-aged obese men. Int J Obes Relat Metab Disord, 1992. 16(12): p. 991-7.
31. Baumgartner, R.N., et al., Imaging techniques and anatomical body composition in aging. J Nutr, 1993. 123(2 Suppl): p. 444-8.
32. Kuk, J.L., et al., Age-related changes in total and regional fat distribution. Ageing Res Rev, 2009. 8(4): p. 339-48.
33. Huffman, D.M. and N. Barzilai, Role of visceral adipose tissue in aging. Biochim Biophys Acta, 2009. 1790(10): p. 1117-23.
34. Chang, S.H., et al., A systematic review of body fat distribution and mortality in older people. Maturitas, 2012. 72(3): p. 175-91.
35. Tchernof, A. and J.P. Despres, Pathophysiology of human visceral obesity: an update. Physiol Rev, 2013. 93(1): p. 359-404.
36. Kuk, J.L., et al., Visceral fat is an independent predictor of all-cause mortality in men. Obesity (Silver Spring), 2006. 14(2): p. 336-41.
37. Enzi, G., et al., Subcutaneous and visceral fat distribution according to sex, age, and overweight, evaluated by computed tomography. Am J Clin Nutr, 1986. 44(6): p. 739-46.
38. Finelli, C., et al., Should visceral fat be reduced to increase longevity? Ageing Res Rev, 2013. 12(4): p. 996-1004.
39. Forbes, G.B. and J.C. Reina, Adult lean body mass declines with age: some longitudinal observations. Metabolism, 1970. 19(9): p. 653-63.
40. Bhasin, S., et al., Older men are as responsive as young men to the anabolic effects of graded doses of testosterone on the skeletal muscle. J Clin Endocrinol Metab, 2005. 90(2): p. 678-88.
41. Kyle, U.G., et al., Age-related differences in fat-free mass, skeletal muscle, body cell mass and fat mass between 18 and 94 years. Eur J Clin Nutr, 2001. 55(8): p. 663-72.
42. Lee, S.J., et al., Relation between whole-body and regional measures of human skeletal muscle. Am J Clin Nutr, 2004. 80(5): p. 1215-21.
43. Yuki, A., et al., Relationship between low free testosterone levels and loss of muscle mass. Sci Rep, 2013. 3: p. 1818.
44. Wannamethee, S.G., et al., Decreased muscle mass and increased central adiposity are independently related to mortality in older men. Am J Clin Nutr, 2007. 86(5): p. 1339-46.







